
Carefully monitoring the progression of your glaucoma is a significant step in preventing vision loss. Subtle changes that occur in the eye which may not be noticeable to you, must be detected promptly to prevent vision loss. As a patient of the Glaucoma Program at Tyson Eye, you may be asked to return to see your doctor every three months, depending on your stage of glaucoma. At these visits, different diagnostic tests will be performed and compared to the results of your previous tests. These tests are done using state-of-the-art equipment, most of which is computer assisted and capable of providing greatly detailed information about the health of your eyes and your optic nerves. The Tyson Eye Glaucoma Program is a recommended plan to monitor the progression of glaucoma. It is similar to the programs at most major university eye departments.
As a glaucoma patient at Tyson Eye, you are one of many patients that are part of a structured Glaucoma Program in Southwest Florida. We understand the importance of preserving your precious vision and want to do everything in our power to help you escape the damage caused by “the silent thief of sight,” also known as glaucoma.
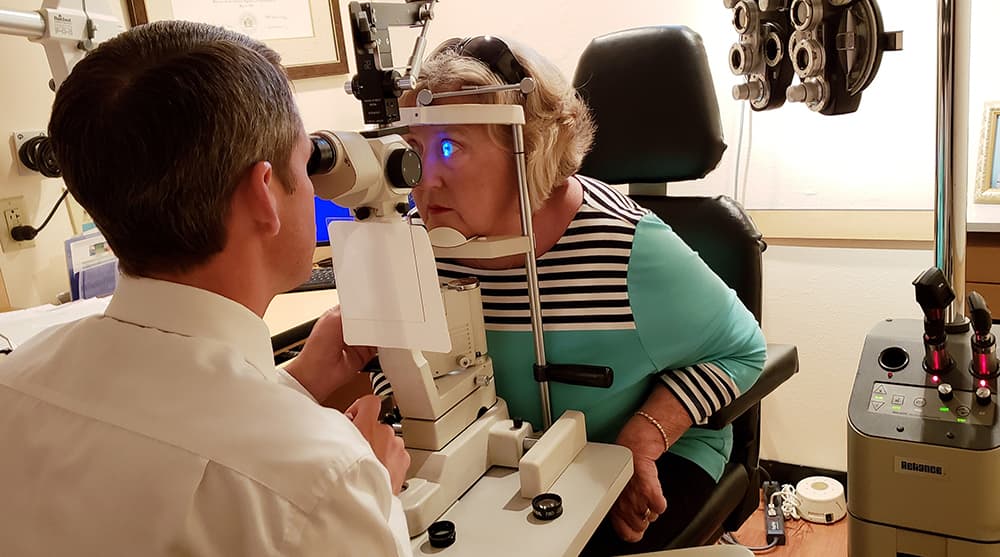
(Based on programs at major university eye departments)
Quarter 1
Comprehensive Eye Examination (including refraction)
Fundus Photos
Quarter 2
Pressure Check
Visual Field Exam Gonioscopy
Quarter 3
Pressure Check
Ocular Blood Flow Analysis
Quarter 4
Pressure Check
GDX or OCT
Eye drops can be used effectively to help maintain and keep your eye at a healthy eye pressure and are an important part of the treatment routine for most people with glaucoma. A variety of glaucoma eye drops are now available by prescription that either increase the drainage of the aqueous humor or slow its production. Sometimes a combination of eye drops is prescribed to obtain the best results.
Various lasers are available to treat the different types of glaucoma. In the United States, laser treatment is growing in popularity as the primary treatment for glaucoma, even over eye drop medications. In many cases, it reduces or eliminates the need for daily drops, a necessary daily ritual that many find expensive and undesirable.
Dr. Tyson and Dr. Stephens specialize in the treatment of glaucoma through minimally invasive glaucoma surgery (MIGS) which are designed to manage glaucoma in a safer and more natural way than other glaucoma treatments. MIGS treatments can also reduce the dependence of medicated eye drops, benefiting the patient by saving money over time and having fewer daily interruptions to apply eye drops. There are a number of MIGs devices that your surgeon can choose from depending on the characteristics of your eyes.
Seldom used today due to new advances in laser treatment for glaucoma, these traditional surgical procedures are usually turned to as a last resort when all other treatment methods have failed to slow the progression of the glaucoma. These surgical procedures must be done in an operating room under sterile conditions to minimize the risk of infection and complications.